Tips and Tricks for difficult venous access
Troubleshooting – Venous Access
Troubleshooting in Venous Access
Although looks trivial, venous access is the most trickiest part of a pacemaker implantation. The biggest acute morbidity of a pacemaker implantation – a pneumothorax is related to punctured venous access and therefore its not surprising that a large number of centers still practice the method of venous cut-down !
Additionally, one must ensure that longevity of the lead and system are not compromised by a misplaced entry point (e.g. a very medial puncture)
If no access is gained after few attempts, a venogram should be done to delineate the venous anatomy. Persisting on attempting without a visual anatomical clue increases the risk of penumothorax. This is especially true for implanters who are in their learning curve – doing a venogram trains the operator on the correct orientation.
The important points are to advance in fine steps with gentle suction and as soon as blood is seen to stop advancing and aspirate. (With experience, the operator will feel a characteristic giveaway when entering the vein). When advancement is done with fine steps, even in the event of a pleural breech one will not have advanced too much into the lung space thus minimizing depth of lung penetration (air would be aspirated if the lung substance was breached). The parietal pleura is very pain sensitive (via intercostal nerves) and our initial local anesthesia generally does not anesthetize this. Therefore if a giveaway occurs with sharp pain, immediately withdraw the needle as this may be a pleural breach. Soft tissue, vessels (and even the rib periosteum !!) are relatively pain insensitive.
Potential Issues in a difficult venous access
The key issue in puncturing the axillary vein is correct judgment of depth. Vast majority of patients, keeping the angle of entry around 30 – 45 degrees to the skin will be successful.
But in an occasional patient, the vein may not be punctured even when radiographically (AP) seen to be in a satisfactory location. The problem is in our standard AP position, we are unable to judge the depth of the needle (i.e. distance from the pleural border to prevent a lung puncture).
In such case, rotation of the camera to caudal position at 25 – 30 degrees will show the distance between the needle and the plueral border as the x-ray beam is now almost parallel to the plueral surface. A case series by Felix Yang et. al., illustrated this principle and the author has found it to be very useful in cases where depth must be carefully assessed. We don’t do it routinely as this view distorts perception of standard anatomy but very useful when depth has to be gauged after correct direction has been ascertained by AP view.
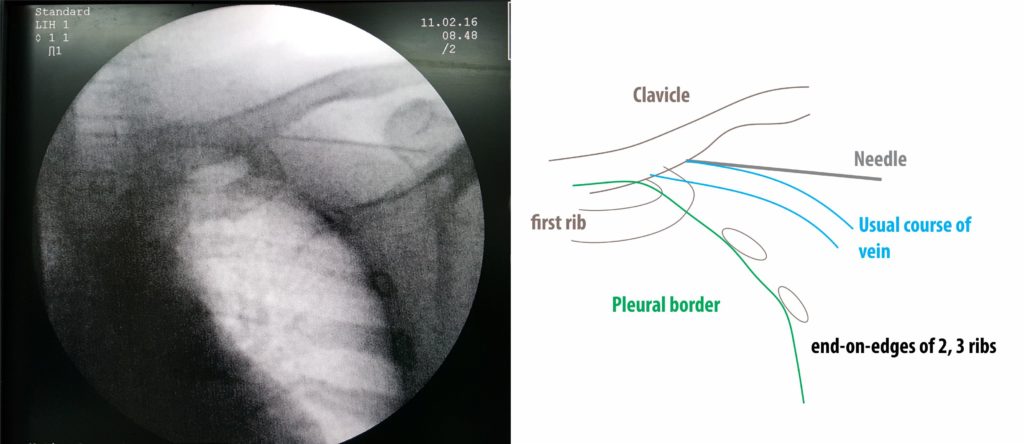
Figure : Fluroscopic view of caudal (35 degrees). If one pauses to think about the x-ray camera’s view point, it would be obvious that the camera is viewing along the anterior surface of the thoracic cage, thus, giving and idea about the depth of the needle (i.e. distance from rib cage to surface). The vein courses “above” the rib cage surface to reach the underside of the clavicle. Ribs tend look end-on in this view and the best judgment of the pleaura is the radiolucent (white) boundary of the lung it self. Therefore as long as one refrains from getting below the white lung margin, he can try various depths to reach the vein. The usual course of the vein is given in the schematic – but if necessary this can be visualized by a venogram.
For the average person, the length of the puncture needle is more than adequate to reach the vein. Upon continuous pushing of the needle in the absence of blood, three things can occur: the needle might hit a bony point (clavicle, first rib or sternum), the needle shaft length may appear inadequate or the needle might pierce the lung.
If it’s the second situation it is most likely that the depth is at issue – pull the needle back while aspirating as at times the needle does a wall to wall puncture of the vein but fails to aspirate as the vein has collapsed – If this was the case, during withdrawal blood is suddenly aspirated thereby confirming position in the vein. If no blood is aspirated while withdrawing, the repeat attempt should aim for a different depth. Same if the needle hits a bony point.
Caution : Longer vascular needles (e.g. B-Braun’s arterial puncture needle) are helpful for very obese patients when the standard needle is about 5 mm shorter. However these needles are super sharp and one may easily enter the lung without noticing.
If air bubbles are aspirated, if the patient suddenly starts coughing or there is sudden pain, the possibility lung puncture should be entertained. The needle should be completely withdrawn and the patient should immediately receive high concentration (>60 %) oxygen to minimize the chance of developing a pneumothorax (Caution in giving oxygen to COPD patients – ironically these patients are the most likely to sustain lung injury as their lungs are hyperexpanded)
If pneumothorax is suspected but there is no clinical evidence (e. g. no patient distress, no de-saturation) one may proceed again but should have a low threshold to call for expert help if there is any further difficulty. At the end of the procedure, continuous screening of upper lung border during a respiratory cycle will reveal pleural separation with air if any significant air leak has occurred. In any case if a pleural breach is suspected, supplemental high flow oxygen is recommend until a definitive CXR is taken post operatively.
Pneumothorax is a occupational hazard for pacemaker implanters and therefore suspicion, identification and management of a pneumothroax is an essential skill to have. More information is available here on the BTS guideline (Note this guideline applies to spontaneous pneumothoraces hence certain long-term planning issues (e.g. driving) may not be applicable to an iatrogenic pneumothorax during a pacemaker implantation
If one attempts vascular punctures regularly, an arterial puncture is bound to happen. Bright red pulsatile flow noted when aspirating blood indicates an arterial puncture. Automatic backward displacement of the plunger or spurts of blood from the needle virtually confirms arterial access and the needle should be withdrawn immediately and firm finger pressure applied to the area for few minutes to seal off the puncture.
If in any doubt whether it is arterial or venous it’s always better to withdraw and do a fresh puncture. Rarely it may not be apparent whether the puncture is arterial or venous (e. g. due to vessel disease, systemic desaturation) and in that case the wire can be gently inserted and guided distally to see where it ends up – if the wire is seen descending on the left side of the spine below the diaphragm, then its arterial (e. g. wire in aorta). If the wire is on the right side of the spine below the right atrial silhouette (i. e. wire in IVC) then its venous. A very rare except for the lead to go down on the left side would be a persistent left SVC. However the guide wire will be seen ‘crossing’ the mid-line just above the diaphragm to enter the right atrium via the coronary sinus. A wire in the Aorta / LV will not cross in such manner. If one is very sure that the wire is in a left SVC the next step would be to inject a good bolus of contrast from the cannula and do a long venogram to track the contrast flow into the left SVC. Wire and contrast flow in the same path confirms the presence presence of a left SVC and the wire in it.
If a sheath is passed in to the artery, and this fact is realized when attempting to send the lead in, one should not remove the arterial sheath. The dilator assembly and guide-wire must be re-inserted thru the sheath and urgent surgical opinion sought. Complete removal of sheath will leave a 7 / 8 Fr hole in the artery which may not compressible and lead to catastrophic bleeding.
First of all – it should attempted by an experienced operator. A preprocedure venogram is helpful. If one finds that the needle length is not adequate for standard axillary vein puncture there are four options available. They are given below in the order of least desirable on top.
- Attempt a very medial sublcavian puncture : This technique generally works but at a greatly increased risk of pnemothorax and long term lead issues. therefore its should be a last choice.
- Attempt with a longer needle – Again the actual length differences are small and in relative terms, the longer needle may not be adequate. Furthermore longer needles have very sharp tips that can lead to an inadvertent pneumothorax in a already difficult patient.
- Do a cephalic cutdown – The old and very safe technique of vascular access. However, in Asians, venous cut downs can be messy as veins are tiny and if multi lead devices are planned, the vein may be inadequate (this is the safest option if one is proficient in venous cutdowns).
- Make the pocket and puncture through the pocket. – If the venogram is satisfactory, one can make the pocket and attempt puncture through the floor of the pocket. Usually when once on the pocket floor, the vein is just adjacent and needle length will not be a problem. This is the authors’ preferred method of access in obese patients – however it assumes that the operator is proficient in puncturing through the pocket. To gain that proficiency, one can practice on regular patients who undergo venography by making the pocket and puncturing through the pocket.
Wrap-up : Workflow guide for vein access
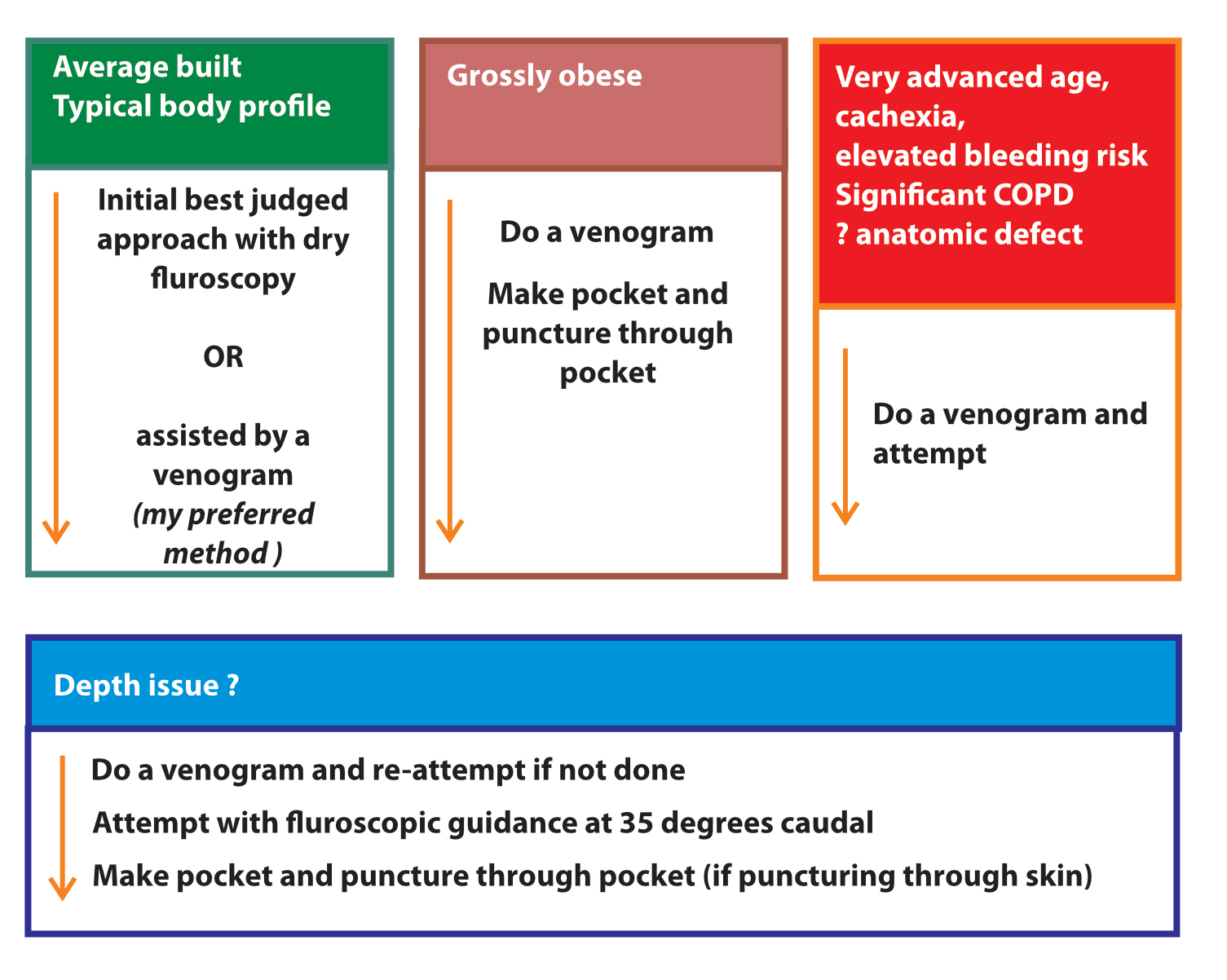
Figure : The venous puncture workflow cascade. With experience, the operator can get venous access easily. In a vast majority of patients, access succeeds in 1 to 3 attempts. The key is anticipating difficulty before attempting a puncture. Low BMI, female sex, COPD, age > 80, dual chamber device are risk factors(1) for a pneumothorax and a low threshold for radiologic aid (venography or ultrasound) should be the norm for these patients. Persisting without a radiologic aid is asking for trouble. Always try to access the axillary vein rather than the subclavian vein and if a venogram is done, use it to guide the punctures – especially in multi lead devices. (The role of the venogram is to guide the puncture at the best location – not to merely reassure the presence of the vein and attempt randomly!).
Note on venous cutdowns : The author has minimal experience in cutdowns (there had been no necessity for a cutdown in the recent past in author’s institution). However it may be the best option to chose in the hands of an experienced cut-downer when punctured access becomes difficult
Further Reading :